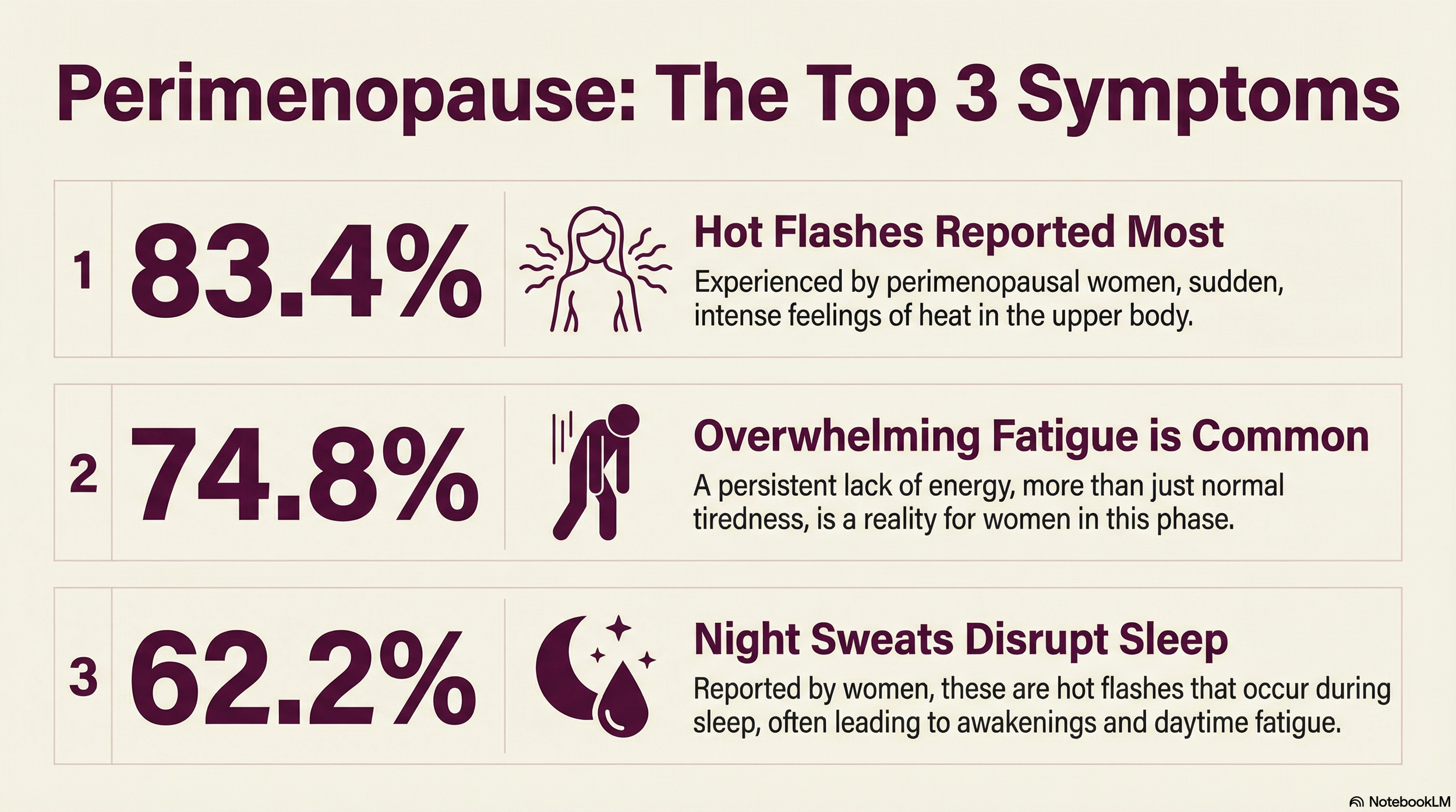
What are Perimenopause Symptoms?
Quick definition
Perimenopause is the "storm before the calm." It's the transitional phase leading up to menopause (the day you've gone 12 full months without a period). While menopause is a destination, perimenopause is the journey, and for many of us, it's a bumpy ride. It's marked by wild fluctuations in hormones like estrogen and progesterone. For Black women, this transition often starts earlier (sometimes in the late 30s) and the perimenopause symptoms can last longer (up to a decade).
What it can affect in real life
It's not just about hot flashes. It's about how you show up in the world.
The "Ambition Tax" at Work: Brain fog and fatigue can make high-performing women feel like they're losing their edge. You might fear speaking up in meetings because you can't find the right word, or worry you'll be seen as incompetent.
The "Sandwich" Squeeze: This often hits right when we're caring for aging parents and raising children. The physical exhaustion makes this "club sandwich" generation role feel impossible sometimes.
Relationships: A drop in libido (sex drive) or a spike in irritability can cause friction with partners. The "people-pleasing collapse" is real. You may find you suddenly have zero patience for carrying the emotional load for everyone else.
What it can look like day to day
Symptoms don't happen in isolation. They often show up in clusters.
The "Internal Furnace": You might wake up drenched in night sweats or feel sudden, intense heat during the day. For Black women, these are often more frequent and intense.
The "Cycle Chaos": You may experience perimenopause irregular periods. One month is "flooding" (soaking through protection in an hour), the next month is skipping entirely, or the cycle length keeps changing.
The "Brain Drain": If you're asking what does brain fog feel like, it often feels like walking into a room and forgetting why, or struggling to find simple words. It's not dementia. It's hormones.
The Emotional Rollercoaster: You might feel a sudden spike in perimenopause anxiety or rage that feels chemical rather than situational. It feels like your emotional footing is shifting.
The Body Shifts: Joint pain, heart palpitations, itchy skin (formication), and weight gain around the middle that won't budge with your usual tricks.
Why it happens (plain-English biology)
Your ovaries are winding down, but they aren't doing it gracefully. Instead of a slow slide, your hormones are on a rollercoaster.
Estrogen Chaos: Estrogen doesn't just control periods. It helps your brain use energy. When estrogen levels fluctuate, your brain experiences a "brownout." It struggles to get the glucose (sugar) it needs for energy. This causes the brain fog and mood swings.
The Cortisol Spike: This transition puts stress on the body, raising cortisol (stress hormone) levels. This can make you feel "wired but tired" and disrupt your sleep even more.
The "Weathering" Effect: For Black women, the biological impact of dealing with systemic racism and chronic stress (weathering) can accelerate biological aging, leading to earlier and more severe symptoms.
What helps (Tier 1, 2, 3)
Tier 1: Lifestyle (The Daily Non-Negotiables)
Stabilize Blood Sugar: Eat protein and fiber every 3 to 4 hours. This stops energy crashes that mimic hormonal dips.
Prioritize Sleep Hygiene: Keep the room cool and dark. Sleep is when your brain "cleans" itself. Avoid screens an hour before bed.
Lift Heavy Things: Strength training is essential right now to protect bones and metabolism. It's often more effective than aggressive cardio, which can spike cortisol.
Tier 2: Supplements (The Support Crew)
Magnesium Glycinate: A go-to for sleep, anxiety, and muscle relaxation.
Creatine: Not just for bodybuilders. It supports brain energy and muscle retention.
Vitamin D: Critical for bone health, especially as estrogen declines.
Omega-3s: Good for brain health, joint pain, and inflammation.
Tier 3: Medical Support (The Heavy Lifters)
Menopause Hormone Therapy (MHT): (Formerly HRT). Replaces the hormones your body is losing. It's the most effective treatment for hot flashes and night sweats.
Non-Hormonal Options: SSRIs (antidepressants) or new medications that block hot flash signals in the brain.
Vaginal Estrogen: A localized treatment for dryness and painful sex that doesn't affect the whole body.
Tools and resources
The Menopause Society (formerly NAMS): Use their "Find a Practitioner" tool to locate a certified expert.
Black Women's Health Imperative (BWHI): Resources specifically for navigating health equity and finding culturally competent care.
Symptom Trackers: Apps like Natural Cycles by Oura can help you log symptoms to show your doctor.
Workplace Accommodations: You can ask for "reasonable accommodations" like desk fans, flexible start times, or camera-off breaks during virtual meetings.
You don't have to "tough it out."
When to talk to your doctor
Don't suffer in silence. See a doctor if:
Bleeding is scary: You're soaking through a pad/tampon in an hour or bleeding for more than 7 days.
Mood is unmanageable: You feel a level of rage, anxiety, or depression that feels unsafe or completely out of character.
Life is disrupted: You're considering quitting your job or your relationships are suffering due to symptoms.
Advocacy Tip: If a doctor dismisses you, say: "My symptoms are interfering with my ability to work and function. I would like to rule out hormonal causes. If you're refusing to test or treat, please document in my chart that I asked and it was declined."
Tracking prompts
Doctors love data. Before your appointment, track at least 2 of these for 4 weeks:
Cycle: Start date, end date, and flow intensity (spotting vs. flooding).
Heat: How many hot flashes or night sweats per day?
Brain: Rate your brain fog or focus on a scale of 1 to 10.
Mood: Did you feel rage, tears, or high anxiety today?
Related terms
Flooding: Shockingly heavy bleeding where you soak through protection in an hour or pass clots.
Dyspareunia: Painful sex, often caused by thinning vaginal tissue and dryness during perimenopause.
Window of Vulnerability: The phase where hormone fluctuations mess with your brain's mood regulation, raising your risk for new or worsening anxiety and depression.
Super Flashers: Women who start having hot flashes well before their periods stop and continue having them for years into post-menopause.
FAQs
Q: Is it Perimenopause or ADHD? A: It could be both. Low estrogen impacts dopamine (the focus chemical). This can make existing ADHD worse or make you feel like you suddenly developed it in your 40s.
Q: Can supplements fix everything? A: Supplements like black cohosh or red clover can help some women, but they aren't miracle cures. They work best when combined with lifestyle changes.
Q: Why does it feel like I'm going crazy? A: You aren't. Your brain is recalibrating to a new normal. The "window of vulnerability" for depression and anxiety is higher right now, but it's treatable.
Research Transparency & Methodology
I believe that every woman deserves health information rooted in evidence, not just social media trends. To ensure clinical accuracy, the content on this site is developed using a dedicated research workspace where I synthesize data from high-authority medical sources, including:
Longitudinal Studies: Data from the Study of Women’s Health Across the Nation (SWAN), a 25-year multi-racial cohort study tracking the physical and emotional changes of the menopause transition.
Clinical Standards: Official position statements and guidance from The Menopause Society (formerly NAMS) and the International Society for the Study of Women’s Sexual Health (ISSWSH).
Neurological Research: Peer-reviewed studies on brain health and metabolism, including the work of leading neuroscientists like Dr. Lisa Mosconi.
Equity-Focused Data: Insights from the Black Women’s Health Imperative (BWHI) and research on the "weathering hypothesis" to address the specific health disparities faced by Black women in midlife.
My Goal
I do the "heavy lifting" of reviewing research so you can stop second-guessing your symptoms. By putting clinical language to your lived experience, I aim to provide you with the tools necessary to advocate for yourself in the healthcare system and get the care you deserve.
Disclaimer: I am not a doctor. This information is for educational purposes only and does not substitute for professional medical advice. Always consult with a healthcare provider regarding your specific health needs.